Obesity Therapy – A New Perspective
Obesity Therapy - A New Perspective
Author: Mark Parkinson RPh: President AFC-CE.com
Credit Hours 1.5 - Approximate time required: 90 min.
Educational Goal:
To give Adult Foster Care providers an update perspective on the management of obesity.
Educational Objectives:
- Define obesity.
- List the contributing factors that lead to obesity
- Explain about the therapeutic options for the management of obesity
- Present caregiver concerns about obesity management and list helpful hints
Procedure:
1. Read the course materials. 2. Click on exam portal [Take Exam]. 3. If you have not done so yet fill in Register form (username must be the name you want on your CE certificate). 4. Log in 5. Take exam. 6. Click on [Show Results] when done and follow the instructions that appear. 7. A score of 70% or better is considered passing and a Certificate of Completion will be generated for your records.
Disclaimer
The information presented in this activity is not meant to serve as a guideline for patient management. All procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this article should not be used by care providers without evaluation of their patients’ Doctor. Some conditions and possible contraindications may be of concern. All applicable manufacturers’ product information should be reviewed before use. The author and publisher of this continuing education program have made all reasonable efforts to ensure that all information contained herein is accurate in accordance with the latest available scientific knowledge at the time of acceptance for publication. Nutritional products discussed are not intended for the diagnosis, treatment, cure, or prevention of any disease.
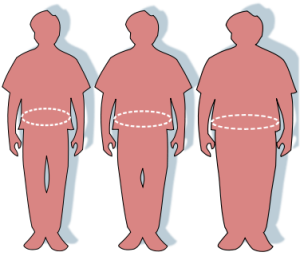
Obesity Therapy - A New Perspective
Throughout the history of mankind, there have been individuals so overweight that it seriously affects their health and wellbeing. Because weight gain in the general populace has always been a matter of choice, it is commonly believed that extremely overweight individuals must have chosen to be that way as well. All that changed in June 2013 when the American Medical Association recognized obesity as a disease state and recommended several medical therapies to treat it. As part of the health care team, adult foster care providers must now recognize obesity as a disease and learn their role in its treatment.
What Is Obesity?
How a word is defined has a tremendous effect on how it is used. Traditionally, obesity has been defined as an abnormal amount of body fat that is at least 20 percent more than an individual’s ideal body weight. That is an extremely basic definition and only defines what obesity looks like, not what it actually is. A more useful definition of obesity is: a multifactorial disease state that leads to an excessive accumulation of body fat that exceeds 20 percent or more the ideal body weight of a patient. This places emphasis on the causes, not the outcome
Causes of Obesity
Obesity is actually a very complex and not-fully-understood condition that leads to being harmfully overweight. At its most basic analysis, weight gain is derived from eating more calories than needed. The excess is converted to fats and stored in adipose cells for later use. If this process continues without the stored fats being used, then a disproportionately large amount of adipose tissue is created and obesity occurs. Why the process continues into the unhealthy state of obesity is not fully understood and is probably caused by many factors.
Contributing Factors That Lead to Obesity
Research is being conducted on the causes of obesity, and new discoveries contribute to our understanding of the disease. While not all causes have been discovered, it is clear is that each obesity sufferer has his or her own collection of contributing factors that lead to being extremely overweight. Some factors are under the patient’s control and some are not.
Voluntary Factors
Diet- There is a lot of controversy about which collection of foods leads to obesity. High-calorie and high-fat-content foods certainly are more easily converted into excess fat than others. But a diet is more than a collection of foods. Diets are formed under the influence of many factors. To truly understand a person’s diet, you must look at the whole person and what motivates them and not just the foods they select. For example, the selection of a deep fried food diet may be the result of cultural influences rather than personal choice based on taste preferences. In such cases, culture is a contributing factor that causes obesity.
Sedentary Lifestyle- An obesity-causing lifestyle is characterized by a lot of sitting and little physical exercise. It is a self-perpetuating contributing factor. The more obese the patient is, the more sedentary they become.
Societal Influences- A person’s motivations cannot be understood without looking at the society they live in. We live in a consumer society in which appetites and desires are boisterously catered to. It is so easy to be swept along the societal current of labor- saving convenience and instant gratification. Appetite control is certainly a lot harder today than in times past.
Food as Therapy- Food or the pleasure we get from food can become a maladaptive response to the stresses of life. We eat because we’re bored, or we eat to unwind from a stressful day. In such cases, the lack of coping skills is the cause of obesity more than the food itself.
Involuntary Factors
Genetics- The genes a person is born with play a significant role in fat accumulation. Genetics influences how appetite is regulated, controls the metabolic rate, sets the homeostasis mechanisms (keeping things the same even if it’s unhealthily heavy), and produces the control mechanisms of the body, including fat-controlling hormones.
Mental Health- Motivations, appetites, and even metabolic rates can be influenced by mental health issues. For example, depression leads to obesity in several ways.
Medication Side Effects- Drugs can have unintended effects on the body and its metabolism that can contribute to weight gain. Medications that can lead to weight gain include older antidepressants, antihistamines, beta blockers, antipsychotics, corticosteroids, certain diabetic drugs, anti-seizure and mood stabilizers.
Other Diseases- Diseases can alter the way our bodies operate, and some effects can lead to excessive weight gain. Hypothyroidism, polycystic ovarian disorder, Cushing’s disease, and uncontrolled diabetes are among the conditions that can contribute to obesity.

Getting a Clearer Picture of Obesity
It should be clear by now that obesity is much more complex than just choosing to eat more than you burn off. It usually is a collection of contributing factors, many of which are lifelong concerns. Just choosing to lose weight is too simplistic an approach and will ultimately fail to be sustainable in the long run. Those who think that the problem will go away once the weight is gone are doomed to disappointment and failure. The weight will come back because the underlying causes where never addressed. Obesity must be viewed as a disease state that has to be actively managed throughout a patient’s life.
Therapy
There is no cure for obesity, but it can be effectively managed. It will be a lifelong struggle but well worth the effort. When managed properly, the emphasis will change from how a person looks to how healthy a person is. Those who can effectively manage their weight will significantly reduce the incidence and severity of type 2 diabetes, heart disease, sleep apnea, arthritis, high blood pressure, gallstones, hernias, heartburn/GERD, skin disorders, and infections. In addition, mental health problems can be reduced with the removal of the negative self-image that obesity inspires. Ultimately it is more productive and sustainable to concentrate on how healthy a patient is not just how thin they are.
How Much Weight to Lose
Getting down to a patient’s ideal weight maybe the ultimate goal, but significant health benefits can be achieved with even a modest weight reduction. Weight loss research has determined that fat associated with vital organs is among the first fat stores to be reduced. So in weight reduction, any weight loss can be beneficial. Recent studies have shown that with a 5-10 percent drop in weight can result in a drop in blood pressure, lower levels of cholesterol, reduction of heart disease, and increased control of blood glucose.
Where to Start
Assessment of the attitudes, motivations, and understanding of all those involved is the first step in therapy. Any successful weight loss plan starts with forming the proper attitude for the patient and caregivers and disregarding false or misleading perceptions.
Properly educating the patient and caregiver is the next step. More effective weight loss efforts stem from a more complete understanding of what obesity really is. A better understanding can lead to more realistic expectations and more achievable goal setting. This resetting of understanding should also extend to the social network and family members of the patient.
In short, obesity management starts with asking questions and searching the answers for misconceptions. Then follow up by educating to change false perceptions. This process should continue throughout the course of therapy.
How Fast Should the Weight Come Off
Rapid weight loss goals are counterproductive. The emphasis of such efforts is on how the patient looks not how healthy they are becoming. They may be very encouraging to the patient but harder to achieve and maintain thus ultimately discouraging to the patient. The National Heart Lung and Blood Institute has recommended the following:
For Adults
•Try to lose 5 to 10 percent of your current weight over six months. This will lower your risk for coronary heart disease (CHD) and other conditions.
•The best way to lose weight is slowly. A weight loss of one to two pounds a week is doable, safe, and will help you keep off the weight. It also will give you the time to make new, healthy lifestyle changes.
•If you've lost 10 percent of your body weight, have kept it off for six months, and are still overweight or obese, you may want to consider further weight loss.
For Children and Teens
•If your child is overweight or at risk for overweight or obesity, the goal is to maintain his or her current weight and to focus on eating healthy and being physically active. This should be part of a family effort to make lifestyle changes.
•If your child is overweight or obese and has a health condition related to overweight or obesity, your doctor may refer you to a pediatric obesity treatment center. ”
Source -http://www.nhlbi.nih.gov/health/health-topics/topics/obe/treatment
How to Lose the Weight
There are thousands of ways to lose weight but most are ineffective at managing obesity. The hallmark of truly effective obesity management addresses the multifactorial causes of the disease.
Effective weight control involves combining multiple techniques and strategies, including dietary management, sustainable physical activity, behavior modification, medications, and even surgery.
Diet
Long-term dietary management is an essential part of obesity therapy. How and why foods are selected, what foods are consumed, and how much is eaten are all important elements of therapy. The long-term goal is to change food from a cause of obesity to a therapeutic tool for greater health. Diets that decrease caloric intake must be able to maintain nutritional values or healthy outcomes will be compromised.
Experts suggest that a negative 500- 1,000 calories difference between what is consumed and what is burned off through activity will help achieve the goal of one-two pounds of weight loss per week.
Physical Activity
Physical activity is an important part of obesity therapy and essential to achieving and maintaining good health. Increased exercise will at first increase weight reduction but taper off as therapy progresses. Despite this, many of the health benefits achieved by increased activity will not reduce over time. There will always be therapeutic benefits to increased activity even if no weight is lost. Increased activity is good for the heart, increases bone mass, maintains balance and coordination, and reduces stress. Increased physical activity can be achieved in everyday routines such as walking instead of riding, doing chores manually instead of using a machine, and gardening. Exercise routines are effective therapy but should be done with caution so they don’t cause harm.
A basic guideline for how much activity to achieve is 30-45 minutes of moderate exercise a day, three to five times a week. Long-term fat stores are most effectively reduced with more than 45 minutes of exercise.
Behavior Modification
Behavior modification is more than just making correct choices. It is rearranging mental thought patterns. Regardless of the cause, obesity sufferers have developed a set mental pattern that helps them cope with the condition. Many of these mental actions actually reinforce obesity-causing choices and thus become maladaptive. If the mental actions occur enough, they become automatic responses without much conscious thought. In certain mental actions involving pleasure, the brain can actually “rewire” its self to always try to get pleasure even if the result is harmful. This is one way to describe addiction: a maladaptive automatic response to pleasure that overrides the choices we make.
Fortunately the mind is changeable. We can consciously override automatic mental responses. If continued long enough, we can “rewire” the brain for the better, but it takes time for that to happen. It takes more than making a few right choices for a couple of months. It is a long-term process that must be maintained in order to rearrange our automatic responses. Changing a single thought is immediate; changing an automatic response (habits) may take years.
The process of behavioral modification can be supported and reinforced by caregivers. Maladaptive responses can be explained for what they really are. Good choices can be praised so that patients can have pleasurable reinforcing responses. Proper education can replace incorrect conceptions, and successful weight loss methodology can replace ineffective short-term thinking. Most importantly, caregivers can help change patients’ thoughts of trying to “cure” obesity by becoming thin to managing obesity to become healthy.
 |
Medications
There is no pill for the ill of obesity. Medications can only modify certain contributing factors that lead to being overweight. They can only be used to support overall weight loss efforts.
Medications approved for weight loss:
|
Name |
Action |
|
sibutramine (Meridia) |
Helps increased satiation (i.e., fullness) No longer marketed in the US because of the possibility of dangerous side effects |
|
orlistat (Xenical)—(Alli) |
Blocks the absorption of about one-third of the fat contained in a meal. |
|
lorcaserin (Belviq) |
Promotes satiation |
|
Liraglutide (Saxenda) |
Involved in appetite regulation |
|
phentermine and extended-release topiramate (Qsymia). |
Suppresses hunger and controls appetite |
|
phentermine (Fastin) |
Suppresses hunger |
Medications not approved for but can contribute to weight loss:
|
Drug Class |
Action |
|
Thyroid replacements |
Increases the metabolic rate of the body |
|
Diabetes Medications |
Corrects improper glucose and fat metabolisms caused by diabetes that contribute to weight gain |
|
Anti-depressants |
Controls the overeating and sedentary lifestyle caused by depression |
|
Anti-seizure |
Weight loss side effect |
Herbals and OTC Remedies
There are numerous products claiming to have weight loss properties, but few have been scientifically verified. They may have some use as a support therapy as prescribed by a doctor. For example, caffeine increases the metabolism in the short term.
Surgery
Bariatric surgery is a type of surgical procedure that alters the upper digestive tract. It differs from liposuction surgery, which removes fat through suction (not commonly used as weight loss therapy) in that it alters the way food is digested.
Weight loss is achieved by severely restricting how much food can be taken in and or rerouting ingested food so that a portion of it is not digested and taken into the blood stream.
Two common examples of bariatric surgery are:
1. Gastroplasty- A constricting band is placed around the stomach or staples are inserted to create a small pouch at the top of the stomach. This severely restricts the amount of food that can be taken in at any one time.
2. Gastric Bypass- A small pouch is created at the top of the stomach by stapling off the rest of the stomach. The pouch is then connected to the far end of the small intestine thus bypassing the areas where most of the food calories are absorbed.
Bariatric surgery is very successful at rapid weight loss and retaining reduced weight over the long run. It is not a cure for obesity, though, and comes with many restricting aspects. It requires a surgical specialist, is expensive, requires lifelong follow ups with the doctor, alters the way a persons can interact with others through food (example holiday dinners and other social events), and comes with many serious surgical and post-surgical risks. It is usually reserved for the extremely obese (100 pounds over ideal weight) who have attempted and failed at other therapies.
Caregiver Factors in Obesity Management
Obesity is a serious impediment to the health and contentment of the residents under your care. Diet and lifestyle choices have a major influence on the disease and are a major focus of therapy. There is no other member of the health care team that has greater day-to- day influence on these factors than adult foster care providers. With the right perspective about obesity as a disease, practicing good everyday caregiving techniques and maintaining contact with the rest of the care team, obesity can be successfully managed.
Proper Perspectives
Caregivers must remember that:
- Obesity is more than just eating more calories than you burn off. It is a disease state that has several causal factors that have to be managed.
- Being healthy is the goal of therapy. Being thinner is just a means to an end.
- Management of obesity is more a matter of skill power than a matter of will power.
- Some people will never be thin, but everyone can work toward being healthy.
Important Weight Loss Topics
Homeostasis- The body is built to remain the same. There are powerful metabolic mechanisms that work hard to keep the body within a range of behaviors that it normally operates under. When the resident loses weight, the body will fight to retain the weight. Some of these metabolic mechanisms are long-term processes that are designed to regain weight once it’s lost. Studies have shown that obese patients commonly regain weight that is lost.
Caregivers can help fight these trends by adopting a lifelong attitude of disease management, focusing on health outcomes and continuing efforts even if some weight is regained.
Maladaptive Behaviors- Each obese patient has developed behaviors that enable them to cope with the stress of being overweight. Many are maladaptive responses that only perpetuate the condition. In addition, it is a normal human trait to resist change. Short-term choices to change activities can easily be overridden by long-term habits and entrenched attitudes.
Caregivers can help by educating the patient to replace misconceptions with accurate facts. Help the resident find new ways of coping that do not involve eating more food. Ensure doctor’s orders are followed even when the resident resists. Support the development of new habits and generously apply large amounts of patience.
Childhood Obesity- The goal of obesity management changes in adolescents and children from weight loss to reduced rate of weight gain. In essence, you’re attempting to help the child to grow out of being overweight.
Caregivers can use the same overall weight loss therapies used in adult therapies.
- Modify the diet
- Increase appropriate physical activity and exercise
- Reduce time spent in sedentary activities
- Modify maladaptive behavior
At the present, orlistat is the only medication approved for weight loss in adolescents.
Helpful Caregiver Tips
- Goals- Goal setting is a more powerful motivator when done as collaboration among the patient, caregivers, and doctor. Set small realistic goals. Setting goals in other areas besides pounds lost can help change the resident’s focus to healthy outcomes.
- Record keeping- Keep records of weight loss activities. It is a good way to maintain focus on weight loss efforts. It helps coordinate and communicate with the doctor and helpful in achieving goals.
- Daily check-off lists help establish habits and sustain motivation.
- Therapy diaries can also be a useful tool.
- Water before meals- Drinking water before a meal helps weight loss efforts. In a recent study, 48 adults aged 55-75 years with a BMI of 25-40 kg/m2, those who consumed 500 mL of water prior to each daily meal had a 44 percent greater decline in weight over 12 weeks
- Plate size- Changing plate sizes from 12 inch to 8 inch makes smaller food portions look larger.
- Include family and friends in weight loss efforts. Communication is key to gaining their support.
- Pedometers are a great way to measure increased daily activity and fight the sedentary lifestyle that contributes to weight gain.
- Find rewards other than food. Find out what other things the patient enjoys and substitute them into the patient’s coping strategies. Examples are movies, music, and massages.
- Diabetic diets are also useful for weight loss.
- Changing surroundings helps break habits. Look for things that contribute to eating or sedentary lifestyles and change them.
Weight Loss Terminology
- Adipose tissue — Fat tissue.
- Bariatrics — The branch of medicine that deals with the prevention and treatment of obesity and related disorders.

- BMI — Body Mass Index. A measurement derived by dividing a person’s height in meters by weight in kilograms. A key measurement in obesity therapy.
- Lipids — Another term for fats, specifically an organic molecule made up of fatty acids.
- Hyperlipidemia — Abnormally high levels of lipids in blood plasma.
- Hyperplastic obesity — Excessive weight gain in childhood, characterized by the creation of new fat cells.
- Hypertrophic obesity — Excessive weight gain in adulthood, characterized by expansion of already-existing fat cells.
- Ideal weight — Weight corresponding to the lowest death rate for individuals of a specific height, gender, and age.
Conclusion
Weight loss in extremely overweight individuals has change dramatically with the realization that obesity is a multifactorial disease state and not just a consequence of a lifestyle choice. With this realization the goals of therapy have changed from a onetime event of dieting to become thin to a more comprehensive long-term management of contributing factors that have led to obesity. Being healthy has replaced being thin as the ultimate goal of therapy.
Caregivers can contribute significantly to therapeutic efforts by helping their residents maintain a proper diet, reduce sedentary lifestyle choices, and support weight loss efforts through a variety of ways. Changing the emphasis of therapy from being thin to being healthy will greatly contribute to the wellbeing of those suffering from obesity.
As always, good luck in your caregiving efforts
Mark Parkinson RPh
References:
1. Osama Hamdy, MD, PhD. Obesity Treatment & Management. Medscape.co. Aug. 25 2015 http://emedicine.medscape.com/article/123702-treatment
2. Robert Kushner, MD, Jennifer Costello, PharmD, BCPS, BC-ADM. The Pharmacist's Role in Obesity Management: A Long-term Commitment to Improving Overall Health. PowerPak CE Oct. 10 2013
http://www.powerpak.com/course/content/109485
3. Obesity Treatment. University of California San Francisco Medical Center http://www.ucsfhealth.org/conditions/obesity/treatment.html
4. How Are Overweight and Obesity Treated? National Heart Blood and Lung Institute. National Institutes of Health. Jul 12 2013 http://www.nhlbi.nih.gov/health/health-topics/topics/obe/treatment
5. Gary D Foster, Angela P Makris, Brooke A Bailer. Behavioral treatment of obesity. American Journal of Clinical Nutrition, American Society for Clinical Nutrition. Am J Clin Nutr July 2005 vol. 82 no. 1 230S-235S
http://ajcn.nutrition.org/content/82/1/230S.full
6. Anthony N. Fabricatore, PhD, Thomas A. Wadden, PhD. Treatment of Obesity: An Overview. Clinical Diabetes, American Diabetes Association, Clinical Diabetes April 2003 vol. 21 no. 2 67-72
http://clinical.diabetesjournals.org/content/21/2/67.full
7. The Practical Guide Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. National Heart Blood and Lung Institute. National Institutes of Health. NIH Publication Number 00-4084 October 2000
https://www.nhlbi.nih.gov/files/docs/guidelines/prctgd_c.pdf
8. Obesity. Medical Dictionary The Free Dictionary by Farlex http://medical-dictionary.thefreedictionary.com/obesity
9. Leigh Anderson, PharmD.,Can Prescription Drugs Cause Weight Gain? Drugs.com Feb. 24 2014 http://www.drugs.com/article/weight-gain.html
@@@@@@@@@@Exam Portal
click on [Take Exam]
Purchase membership here to unlock Exam Portal.
|
|
|
|
|
*Important*
Registration and login is required to place your name on your CE Certificates and access your certificate history.
Username MUST be how you want your name on your CE Certificate.
| Guest: Purchase Exam |


