My Journey into the Serious Situation of Cirrhosis
My Journey into the Serious Situation of Cirrhosis
Author: Mark Parkinson BsPharm: President AFC-CE
Credit Hours 3 - Approximate time required: 180 min.
Educational Goal:
Show how to care for Cirrhosis patients and how to handle difficult situations by telling the story of how my wife was diagnosed with Cirrhosis and how I handled the situation.
Educational Objectives:
- Define Cirrhosis
- Explain the causes of the condition.
- List the signs and symptoms.
- Tell how Cirrhosis is diagnosed.
- Show how the seriousness of the condition is determined
- List therapeutic options.
- Explain about the complications that can arise.
Procedure:
Read the course materials. 2. Click on exam portal [Take Exam]. 3. If you have not done so yet fill in Register form (username must be the name you want on your CE certificate). 4. Log in 5. Take exam. 6. Click on [Show Results] when done and follow the instructions that appear. 7. A score of 70% or better is considered passing and a Certificate of Completion will be generated for your records.
Disclaimer
The information presented in this activity is not meant contraindications may be of concern. All applicable manufacturers’ product information should be reviewed before use. The author and publisher of this continuing education program have made all reasonable efforts to ensure that all information contained herein is accurate in accordance with the latest available scientific knowledge at the time of acceptance for publication. Nutritional products discussed are not intended for the diagnosis, treatment, cure, or prevention of any disease.to serve as a guideline for patient management. All procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this article should not be used by care providers without evaluation of their patients’ Doctor. Some conditions and possible
My Journey into the Serious Situation of Cirrhosis
We have all heard of the term Cirrhosis and know it’s a bad thing, but I bet you don’t know much more than that unless you have had medical training. Oh, you might have heard that it has something to do with the liver, and alcoholics get it a lot, so alcohol must be involved somehow. But beyond that, you are most likely clueless. Like I was a couple of months ago, before my wife (who has never had a drop of alcohol in her life) was told by her doctor that her liver was in the early stages of cirrhosis.
You know, being a pharmacist and before that a professional In-home caregiver, I thought I was prepared for anything that a doctor could throw at us. But at that moment, I didn’t know what he was talking about. For the first time in a long time, I struggled to keep up when he started talking about what tests and therapies were going to be needed. I was totally at his mercy and had to just sit there and listen. I didn’t even know enough to ask intelligent questions. I felt incapable of helping or contributing in any way. I didn’t like that one bit. When my wife started to cry a little bit from the fear of the unknown, I got seriously stressed out. I vowed to myself that I would get in the know so I could help. Do you In-home caregivers, sometimes feel that way when you take your clients to the doctor’s office? Kind of like being a third wheel that no one takes seriously? Well, together let’s do something about that. Follow my learning journey to get in the know about liver cirrhosis. Maybe a few pointers will rub off on yah.
My Learning Journey
I started my journey by doing a basic search of medical information sites and continued until I stopped learning new things about the condition. I found out that cirrhosis just means having a scarred liver. So it’s not so much a disease but an end-stage condition of other diseases that affect the liver. Something has damaged the liver so badly that scar tissue has built up to the point where it can’t function properly anymore.
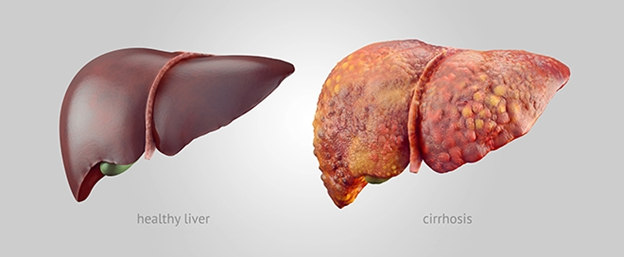
Take a look at these pictures.
On the left is a healthy liver, smooth surfaced and uniform in color. On the right is a liver with cirrhosis.
I thought to myself, “How could this be? I know that since the liver takes care of the damaging toxins the body produces, so it has a tremendous ability to repair itself. What’s going on? Why all the damage?”
It turns out that yes, the liver can repair itself, but everything has its limits. Here’s a simplified blow-by-blow in the fight to repair liver damage.
- When liver cells are seriously stressed, some will start to die.
- The damaged cells leak chemicals that trigger the protective inflammation process in the tissue and also the cellular repair process.
- The normal repair process produces collagen fibers in between layers of healthy liver cells, as a framework for functional tissue regeneration.
- But if damage continues and the liver is forced to repeatedly repair itself, then the fibers start to build up. The tissue becomes fibrotic, and scar tissue is formed. It’s kind of an automatic last-ditch effort to contain the damage. This condition is understandably called Fibrosis.
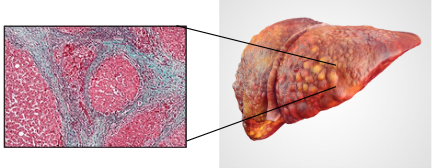
- Unfortunately, the buildup of scar tissue is irreversible. If the process continues, then clumps of healthy functional liver cells are surrounded by scar tissue, and what’s called regenerative nodules are formed. The result is that the liver starts to have a discolored, lumpy appearance. If the condition becomes widespread throughout the liver it’s called Cirrhosis or End-Stage Liver Damage.
The blue-stained area is fibrotic tissue surrounding regenerative nodules.
So on the first step of my learning journey, I found out that Cirrhosis is a chronic progressive condition where scar tissue gradually replaces healthy liver tissue. At first, the liver will be able to work around the scar tissue, and no outward symptoms will be felt. This early phase is called Compensated Cirrhosis (stage 2 liver disease). But when the fibrosis is extensive, it is called Decompensated Cirrhosis (stage 3 liver disease) and outward symptoms that start to show. They are related to the fact that liver can’t do it’s job well.
On to the second step in my learning journey.
How serious is the condition?
What Causes the Damage
Ok, it’s a given that making the liver deal with long-term exposure to toxins (Alcohol, industrial solvents etc…) can cause cirrhosis. But what about my wife, who’s a non-drinker and never worked around a lot of chemicals? I found out that the following can also put long-term stress on the liver.
Common Causes
|
Alcoholic liver disease (ALD, or alcoholic cirrhosis) |
It is seen in 10–20% of individuals who drink heavily for a decade or more. 40% of cirrhosis-related deaths are due to alcohol in the US |
|
Non-alcoholic fatty liver disease (NAFLD)
Metabolically-dysfunction-associated steatohepatitis |
Fat builds up in the liver and eventually causes scar tissue. Fatty liver disease can be caused by obesity, diabetes, malnutrition, coronary artery disease, and Chronic steroid use. |
|
Chronic hepatitis C |
The hepatitis C virus causes inflammation of the liver, which eventually damages the organ. 20-30% of patients with chronic hepatitis C infections develop cirrhosis. Hepatitis C and alcoholic liver disease are the most common reasons for liver transplants. |
|
Chronic hepatitis B |
Chronic hepatitis B also causes liver inflammation and injury. It may take several decades for cirrhosis to develop. Both hepatitis C and hepatitis B–related cirrhosis can also be linked to heroin addiction. |
Uncommon Causes
|
Autoimmune diseases |
The body attacks the biliary ducts that lead to the gall bladder. This backs up pressure in the liver and causes damage. Or lymphocytes attack the liver itself. |
|
Genetic disorders |
Inherited disorders can cause toxic substances to build up in your liver. These include glycogen storage disease, cystic fibrosis and Wilson disease. |
|
Toxic hepatitis |
Liver damage is caused by long-term exposure to certain toxins or medications like paint solvents and common painkillers like NSAIDs, acetaminophen, and illicit drugs. |
|
Hereditary haemochromatosis |
Liver damage is caused by the absorption of too much iron from food that is eaten. |
|
Cardiovascular disease: |
Conditions that cause blood to build up in the liver (congestive heart failure) or that prevent blood from reaching your liver (chronic ischemia) can lead to organ damage. |
I also learned that you can be affected by multiple conditions at the same time, which naturally would speed up the liver damage. After taking several tests, the doctor told us the primary cause of my wife’s condition was her diabetes. We suspected as much but were relieved that there weren’t other liver-damaging effects to be worried about.
Signs and Symptoms
The third step in my learning journey was to cover the signs and symptoms of liver disease. Something that should be of particular interest to caregivers. Remember, it’s not your job to diagnose, but it is your job to be suspicious of conditions that are not normal. Then it is your duty to inform the doctor of your observations and tell the doctor of your concerns. You’re going to see the problem before anyone else does, if you’re observant and know what to look for.
But first, you have to know what normal looks like. In order to know that, you need to be familiar with what the liver does for the body. A subject, unless I am totally off the mark, I’m guessing you haven’t given much thought to, because I hadn’t. Here is what I found in my research.
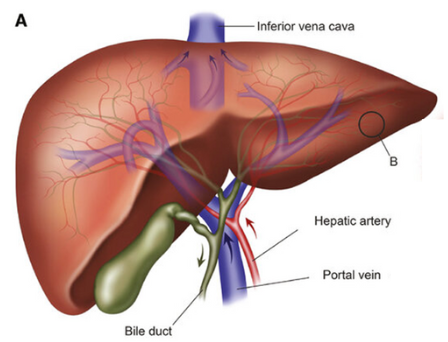
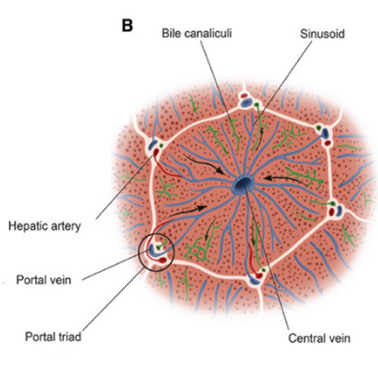
Liver functions include
- Bile production
Bile is a yellow-green acidic liquid that helps carry away waste and break down fats in the small intestine during digestion
- Produces blood plasma proteins
Blood plasma transports blood components (red and white blood cells and platelets), and enables the transportation of nutrients, hormones, proteins, and waste products.
-
- Produces cholesterol and special proteins to help carry fats through the body
- Helps keep steady blood glucose levels. It converts unused glucose into glycogen for storage and converts it back into glucose when it is needed.
- Works by breaking down fats in your blood to produce energy, and if there are too many, they may get stored as extra fat
- Regulates levels of amino acids in blood.
- Makes cholesterol and certain hormones.
- Stores iron processed from old hemoglobin
- Converts poisonous ammonia, made during digestion, to urea
- Processes drugs and breaks down toxins in the blood
- Regulates blood clotting
- Fights infections by making immune factors and removing bacteria from the bloodstream
- Filters out excess bilirubin from the blood
- Regulates blood clotting factors
Advanced info
For those readers who have had medical training, here is a more advanced summary of liver function. For those who haven’t had prior training, still read it. You may not understand everything, but it will still help you get to know some of the medical phrases that come up from time to time. There will be exam questions.
“The liver is the largest gland in the body and is ideally located to receive absorbed nutrients and detoxify absorbed drugs and other noxious substances. It serves as both an exocrine organ and an endocrine organ. The exocrine functionality of the liver is mainly in the synthesis and excretion of bile salts into the common hepatic duct, as well as the conjugation of bilirubin and excretion into the gut. The endocrine functions of the liver include involvement in glycemic control via insulin and glucagon. The liver synthesizes important proteins such as fibrinogen, albumin, prothrombin, and other amino acids and modifies proteins into enzymes and peptide hormones. The liver participates in fatty acid metabolism and synthesizes lipoproteins, cholesterol, and phospholipids. Additionally, it is involved in the metabolism of carbohydrates, which includes storing glycogen and gluconeogenesis. It is also involved in the metabolism of lactic acid and converts ammonia to urea. The liver stores vitamins and minerals such as iron. In summary, the liver is an important mediator from the gut to the blood and plays a vital role in the metabolism of macronutrients, hormones, components of blood plasma, and exocrine and endocrine substances.” Source: National Library of Medicine- Stat Pearls https://www.ncbi.nlm.nih.gov/books/NBK500014/
The liver also contains many enzymes designed to interact with and alter toxins and other harmful substances. This makes them inert or more easily removed from the body. Cytochrome p450 is a cell membrane-bound superfamily of enzymes with many variants (CYP1A2, CYP2C9, CYP2C19, CYP2D6, CYP2E1, and CYP3A4.) These also have a major effect on the medication the patient takes. If taken orally, the medication will first enter the liver, where a portion of the drug will be inactivated or removed. This is called the first pass effect. If the liver is damaged, the first-pass effect will also be changed. Raising concerns about the dosage amounts that are needed by the cirrhotic patient. This creates an increased need for drug effect monitoring.
Whew! That was a struggle. Now where was I? Oh yes, the third step in my knowledge journey. Now that I had a good refresher on how the liver works, I was better prepared to see and understand the signs and symptoms of Cirrhosis.
If you are getting kind of lost in all the details, here is a video produced by the American Liver Foundation that might help keep you on track.
Malfunctioning Livers
You can’t feel the Liver functioning. What you can feel is the consequences of when it’s not working correctly. But your patients may not notice. It takes a long time for scar tissue to build up to the point of causing the signs of Cirrhosis. Initially, the liver will be able to compensate for the loss of function, so the symptoms will probably be mild and general in nature. The condition takes so long to develop that the patient can become acclimated to the dysfunction and does not even notice that the symptoms are getting worse.
Compensated Cirrhosis
- Low energy or feeling tired all the time
- Nausea or loss of appetite
- Weight loss
Many things can cause these symptoms. So look for confirming signs or several signs together before sounding the alarm. Look for;
- Spider angioma or spider nevi. Visible blood vessels that look like spiders
- Palmar erythema, Redness on the palms of your hands
- Abdominal pain in the upper right region.
- Clubbing of the fingers, in which the fingertips spread out and become rounder than usual.
- Pale fingernails, especially the thumb and index finger.
- Pale lines showing on the nails
Decompensated Cirrhosis
- Jaundice (a yellow tint to your skin and eyes) caused by a build-up of bilirubin
- Dark-colored pee and light-colored poop
- Itchy skin (but with no visible rash) caused by toxins building up in the skin
- Small, yellow bumps of fat deposits on your skin or eyelids
- Unexplained weight loss and muscle loss (muscle wasting)
- Hormone problems (Irregular periods, Gynecomastia, Hypogonadism)
- Easy bleeding and bruising
Two advanced cirrhosis-caused conditions are very serious, and I would like to spend some time on them. If you notice them, plus other signs of Cirrhosis, I would consider that an automatic call to the doctor, even the hospital.
Portal Hypertension
The buildup of scar tissue in the liver makes it hard for blood to flow in the portal venous system. The tissues go from being like a sponge to being like a rock. This in-flow resistance creates a backup of blood and increases the blood pressure upstream from the liver.
Portal hypertension causes:
- Swelling in your abdomen (ascites)
- Edema in the legs and feet
- Caput medusae (pronounced blood vessels seen just under the skin.)
- An enlarged spleen
- Esophageal varices (enlarged blood vessels on the inside of the throat)
Hepatic Encephalopathy
Hepatic Encephalopathy literally means liver-caused brain function disorder. When the liver can’t clear blood toxins like ammonia and dimethyl sulfide. They build up and cause harm.
- Dimethyl sulfide, being expelled with the breath, causes Fetor hepaticus (a musty breath odor).
- High ammonia levels cause memory loss, sleep disorders, personality changes, confusion, drowsiness, and slurred speech. It can be a lethal condition if left untreated.
This is what my wife experienced that started this whole journey. She was so mentally dysfunctional, I thought she was having a stroke. I took her to the ER, and they determined that there was no stroke, but noticed on one of their tests that the blood ammonia levels were very high. After that, they kind of just sat on their hands. I had to get very aggressive and demanded that they find out what was going wrong. They reluctantly admitted her to the hospital. I still had to push around some poor nurses to finally get a Doctor who could connect the dots between my wife's high ammonia levels and her mental condition. They gave her Lactulose. A strong laxative of all things. I believe that saved her life.
I know that was a lot of signs and symptoms to handle. You don’t have to memorize them all. You just have to be familiar enough to recognize that something is not normal in your residents. Then call the doctor with your observations and start asking the right questions. Like, how come this and that are happening together? Could it be something to do with liver function problems? I wish what I know now, I knew then, and I wouldn’t have had to be such an aggressive jerk to those hospital nurses. I think the doctors found out that they couldn’t buffalo a grouchy pharmacist and avoided me, but the poor hospital staff were stuck with cranky me.
Here is a good video about liver disease symptoms for all you visual learners out there. There will be an exam question.
Diagnostic Tests
The fourth logical step I took in my learning Journey was to find out about all the tests that my wife undertook.
Boy, there were a lot of them.
In the hospital, blood was taken several times, and a series of tests were administered on the samples. Among those tests was a Comprehensive Metabolic Panel (CMP), which includes a so-called “liver function test”.
The liver function test measures the amount of certain liver enzymes and proteins in the blood. If too much is found in the blood, then something is not right.
- Alanine transaminase (ALT).ALT is an enzyme found in the liver that helps convert proteins into energy for the liver cells.
- Aspartate transaminase (AST).AST is an enzyme that helps the body break down amino acids.
- Alkaline phosphatase (ALP).ALP is an enzyme found in the liver and bones and is important for breaking down proteins.
- Gamma-glutamyl transferase (GGT).GGT is an enzyme in the blood. Higher-than-usual levels may mean liver or bile duct damage.
- L-lactate dehydrogenase (LD).LD is an enzyme found in the liver.
- Prothrombin time (PT).PT is the time it takes your blood to clot. Increased PT may mean liver damage.
- Albumin and total protein. Albumin is one of several proteins made in the liver.
- Bilirubin. Bilirubin is a substance produced during the breakdown of red blood cells.
The Mystery of My Wife’s Test Results
I said, So-called liver function tests, because I found out in my research that a CMD is not very good at telling us how well the liver is functioning. It mainly tells us that the liver cells have been damaged to the point that these enzymes have leaked out into the bloodstream in higher-than-usual levels.
My wife’s CMD showed only that ALT and ALP were slightly higher. Everything else was within normal ranges. I guess that is why they didn’t look too hard at the Liver being the cause of my wife’s mental confusion. Because it appeared from the CMD that the liver was normal. Boy, I’m glad I pushed the hospital staff to look harder into the mystery. After getting in the know about cirrhosis, here is my hypothesis on what happened.
Our liver cells (Hepatocytes) have a tremendous ability to repair themselves. It is only after many harmful events over a long period of time that scar tissue starts to build up, and the fibrosis starts to replace healthy functional cells. So in my wife’s case, there weren’t enough damaged cells to leak enzymes and proteins to abnormal levels. But there were not enough functional hepatocytes to clear the ammonia out of her brain. With the benefit of hindsight, clearly more tests were needed.
Mini-Mental Health Test
The next significant test she was given was administered by the nurses. I think it was given because I kept demanding that they do something about her mental state. They asked her simple questions that normally people would have to think about, but can easily answer. What is the day and year? What city was she from? Who was the President? That sort of thing. Then they asked her to draw a face and a clock, complete with hands and numbers.
She answered the verbal question correctly but very slowly. But the pictures she utterly failed at. That got everyone's attention at the ER (that and my combative attitude), and she was admitted to the hospital. As we waited (very impatiently) for the doctor to arrive, the floor nurse asked her to draw the pictures again. She failed even worse. The nurse then did the Asterixis test (the one from the video where you extended your arms with the palms extended forward). She couldn’t hold the position (just like in the video). They kept both attempts at drawing and showed them to the Doctor when he arrived. The nurse also told him about the Asterixis test. That got his attention, and the doctor finally connected all the dots and ordered the laxative therapy that I believe saved her life. It took a couple of days to clear the ammonia, and she was finally able to go home functioning well mentally. Could you imagine taking a powerful laxative several times a day for several days? Yikes!
I included the story about the mini-mental and the Asterixis tests in this CE because you can do this yourself without a doctor's order, just like the nurses did. You're not determining therapy. You are just making objective observations that you can use to get the doctor’s attention.
Degree of Liver Damage Tests
Both the hospital and my wife’s doctor wanted her to go to a hepatologist (liver specialist). They are also known as gastroenterologists (gut doctors). I found a really good one who advertised himself as the “Gut Whisperer”. It was at his office that I found out just how clueless I was about the liver. He ordered several more tests that I had to do more reading up on to understand what they were for.
By this point, it was pretty much a given that there was something wrong with the liver. The important question was just how bad things were. The doctor already had the liver function test results from the hospital. He now had two more tests he could choose from.
- Elastography
Elastography is a test that uses painless, low-frequency vibrations to check the elasticity of the body’s organs. It measures how stretchy the tissues are. When tissues lack elasticity and are stiff, it may indicate how much fibrosis has occurred. There are two ways to perform the test.
-
- Ultrasound- This is also called transient elastography. It is performed by 1. passing over the abdomen a handheld wand (called a transducer) that emits high-frequency ultrasound waves through the tissue. 2. The soundwaves bounce off different tissues and structures and create echoes. 3. The transducer receives the echoes and translates them into an electric signal that is sent to a computer. 4. The computer compiles the data and creates a picture on a monitor. 5. Interpretation depends on how bright the various tissues show on the monitor. Denser tissues like scar tissue appear more white than normal, blood fluid-filled healthy liver tissues.
- MRE- A magnetic resonance elastography test produces images by combining sound waves from an ultrasound machine and magnetic resonance and radio waves from an MRI machine. It produces more detailed information but is much more expensive and time-consuming.
- Liver Biopsy
A liver biopsy is a procedure where a small piece of the liver is extracted via a needle inserted into the organ. Then the tissue sample can be thoroughly examined under a microscope. It is the gold standard of cirrhosis diagnostic tests. Simple enough to understand, but it’s a bit more complicated when you actually have to do it.
As you would expect, a doctor who called himself the gut whisperer had his own ultrasound machine and was really good a taking liver biopsies. So those were the tests my wife was asked to do. We were relieved because even with insurance, the copay for an MRI would have been hundreds of dollars.
Doing the Exams
The doctor’s staff did the ultrasound right then and there. The sonographer (the person who operates the ultrasound machine) applied some jelly to make the wand move more smoothly over the skin and have better contact for the soundwaves. The jelly was easily cleaned up afterward. The ultrasound images were evaluated right away, confirming that there was fibrosis scar tissue in my wife’s liver. When the doctor tried to explain what that meant, that’s when my wife started to tear up, and I had my “feeling useless” episode. After some calming reassurances and explanations, we set the appointment for the liver biopsy at the hospital.
The day of the liver biopsy, she was told not to eat any breakfast (didn’t want her to throw it up during the procedure). We went to the outpatient surgery department of the local hospital. The doctor had a couple of options on how to perform the procedure. Stick the needle straight in or snake the needle down a large vein in the neck. Since my wife didn’t have a bleeding disorder or ascites (fluid buildup in the abdomen), the doctor chose the simpler straight-in method. She got dressed in a hospital gown, given a shot of anesthesia, and 30 minutes later, it was all done. It took longer for the anesthesia to wear off than for the biopsy procedure. We were given the findings of the biopsy at the next doctor visit. I told those stories, so if your residents ever must have these exams, you will know what to expect and be better prepared to help.
What the Exams Found Out
We went in for the follow-up doctor appointment.
The doctor said a few words to us and turned the case over to one of his Physician assistants. We lucked out and got a PA with a pretty good bedside manner. She told us that my wife’s condition was just over the borderline of decompensated cirrhosis. She also told us a bunch of other things, but since I was still clueless about everything cirrhosis, I left pretty confused and had to deal with a very worried wife. That’s when I got fed up with not knowing and started my learning journey.
The Grading of Cirrhosis
The next step in my learning journey was to understand what the doctor said about how bad my wife's condition was. I learned that the progression of the liver disease is based on how functional the organ remains. It is named either as a stage or its descriptive name. There are four stages.
|
Stage |
Name |
Signs of dysfunction |
|
Stage 1 |
Compensated Cirrhosis |
Liver function is still largely intact. May have no symptoms or mild symptoms such as fatigue, fatigue, and spider veins. |
|
Stage 2 |
Decompensated Cirrhosis |
Liver function begins to decline significantly. Symptoms may include jaundice, ascites, varices, and hepatic encephalopathy |
|
Stage 3 |
Advanced Cirrhosis |
Liver function is severely impaired. Complications such as liver failure, liver cancer, and infections |
|
Stage 4 |
End-Stage Liver Disease |
Liver function is almost completely lost. A liver transplant is required for survival. |
The PA told us the exams showed that my wife was at the border of stage 2, approaching stage three. Now that I understand more about what is going on, I realized she is better off than I originally thought she was.
MELD Score
The next thing the PA talked to us about, which made us concerned at the time, was the possibility of a liver transplant, since that was the only cure for Cirrhosis. As one would imagine, there is always a significant shortage of livers available for transplant. A system had to be developed for how to objectively prioritize who got a transplant when a compatible donor became available. In 2002 MELD (Model for End-Stage Liver Disease) score was approved by the United Network for Organ Sharing (UNOS) for just such a purpose. It is a numerical scale, used for liver transplant candidates aged 12 and older. Children who need a liver go to the top of the list as a matter of course. MELD uses the patient's values for serum bilirubin, serum creatinine, and the INR levels in an equation that results in a score of between 6 and 40. The higher the number, the more serious the patient's prognosis is.
|
MELD Score |
90-day risk of death |
|
Less than 9 |
1.9% |
|
10 to 19 |
6% |
|
20-29 |
19.6% |
|
30 to 39 |
52.6% |
|
Higher than 40 |
71.3% |
The PA told us my wife had a MELD score of 10. Which meant that she was almost at the bottom of the priority list. That concerned my wife. Since then, my research has shown me that the low score was actually very good news. Her liver condition is not as life-threatening as we at first feared it was. Knowing is always better than not knowing.
Now that we have a better understanding of what the Doctor and the Physician's Assistant talked to us about, we are now in a much better position to handle my wife’s condition. Which brings us to the next step in my journey, managing, not curing. Here is what I learned.
No Cure
Why can’t the doctor cure Cirrhosis? Cirrhosis is not a disease in the traditional sense. It is a condition of excessive scarring throughout the liver. There is no homeostatic mechanism to stimulate or medical treatment that reverses the formation of scar tissue. Once it is there, it’s there for good. Also, a doctor cannot remove it by surgically cutting it out because new scar tissue will form in its place. The best that a surgeon could do is reduce the size of the scar tissue. Given how extensively and finely the scar tissue is dispersed throughout the liver, there is no point in even trying. So where does that leave us?
The goal of therapy switches from eliminating the problem to not losing any more of what we got, taking good care of what is left, and compensating for what can’t be done anymore. Broadly speaking, that means reducing what is putting stress on the liver by treating the cause, maintaining proper diet and lifestyle choices, and treating any complications that may arise.
Treating the Cause
- Treat the drug and alcohol addiction- You must control the desire to drink because any amount of alcohol consumed is toxic to the liver.
- Weight loss- Losing weight drops the stress on the liver.
- Control Diabetes- Keeping the A1C down is beneficial to the liver in multiple ways.
- Get treatments to control Hepatitis or other conditions causing liver problems- Ask the doctor for the appropriate medicines, treatments, and vaccinations
Diet and Lifestyle
- Exercise regularly and participate in an active lifestyle
- Maintain a liver-supportive diet with the right amounts of calories, proteins, fats, fiber, and salt.
- Eliminate or reduce alcohol, even if the cirrhosis is not caused by alcohol.
- Report other recurring symptoms that are causing problems. They might be signs related to the cirrhosis condition.
- Supplements may be prescribed to support the liver or make up for what is being lost due to the condition.
Treating Complications and Side Effects of Cirrhosis
- Draining fluid buildup in the abdomen
- Keeping track of Portal Hypertension
- Getting regular vaccinations, like the flu vaccine
- Monitoring for liver cancer, swollen veins in the throat, hepatic encephalopathy caused confusion, jaundice, and internal bleeding.
My wife and I certainly have got our work cut out for us. It’s going to have to be a team effort. Currently, we are looking into the Mediterranean Diet. The doctor also wants her to take extra Vitamin E because of its anti-inflammatory effects and a fish oil supplement to help balance out the good fats and the bad fats in the bloodstream.
In addition, my wife is tired all the time, so my job is being a motivational cheerleader. “Get up out of that recliner and Go team Go”.
Now that we have a better handle on what's going on with her liver, I feel hopeful for a good outcome. I also look forward to being healthier myself; I could stand to lose a few pounds (really more than a few). I plan to continue my learning journey as we discover what works and doesn’t work for maintaining her liver function.
Caregiver Implications
I hope you enjoyed the story of my learning journey. The goal was not only to educate you about cirrhosis but also to give you some practical examples of how to work the medical system for the benefit of your clients. You also now know to screen for those a risk for liver disease. If you catch it soon enough, the liver can heal itself before fibrosis sets in. Those with a history of drug or alcohol abuse, diabetes, obesity, and those developmentally challenged should have their livers examined.
If you do have a client who has been diagnosed with a liver disease or cirrhosis, there is going to be some extra work for you to do.
- The biggest challenge will be the menu. Cooking different meals due to dietary requirements is not fun. Fortunately, a liver-friendly diet is good for everyone. So the easy solution is to put everyone on that diet.
- Because clotting ability is reduced and portal hypertension can cause internal bleeding, you are going to have to monitor for black tarry stools.
- Since a lot of medications are processed in the liver, their concentrations in the patient’s bloodstream may increase. That means a greater chance of side effects. Increase your watch for them, and if they happen, ask the doctor if a dosage change is required.
- Also, schedule regular exercise activities. You know I like those regular resident walks.
Conclusion
For those visual learners, here are two summation videos to watch. (There will be exam questions on them.)
As always, good luck in your caregiving efforts. Mark Parkinson, BsPharm.
References:
- Wikipedia, the free encyclopedia. Dec 6, 2025. https://en.wikipedia.org/wiki/Cirrhosis
- Cirrhosis of the Liver. Cleveland Clinic.org. Last reviewed on 07/18/2025. https://my.clevelandclinic.org/health/diseases/15572-cirrhosis-of-the-liver
- Mayo Clinic.org. Oct. 24, 2025. https://www.mayoclinic.org/diseases-conditions/cirrhosis/symptoms-causes/syc-20351487
- Liver: Anatomy and Functions. Johns Hopkins Medicine 2025. https://www.hopkinsmedicine.org/health/conditions-and-diseases/liver-anatomy-and-functions
- The Healthy Liver. American Liver Foundation. 2025 https://liverfoundation.org/about-your-liver/how-liver-diseases-progress/the-healthy-liver/
- Hamilton Vernon; Chase J. Wehrle; Valentine Sampson K. Alia; Anup Kasi. Anatomy, Abdomen and Pelvis: Liver. NIH National Library of Medicine Stat Pearls. Nov 26, 2022. https://www.ncbi.nlm.nih.gov/books/NBK500014/
- Cleveland Clinic.org Sept 26 2025. https://my.clevelandclinic.org/health/body/21481-liver
- Liver function tests. org. Jan. 18, 2025. https://www.mayoclinic.org/tests-procedures/liver-function-tests/about/pac-20394595
- Cleveland Clinic.org Jun 21, 2022 https://my.clevelandclinic.org/health/diagnostics/23335-elastography
- Liver Biopsy. Cleveland Clinic.org Sept 19, 2023. https://my.clevelandclinic.org/health/procedures/9503-liver-biopsy
- Liver Biopsy. org. Dec. 14, 2024. https://www.mayoclinic.org/tests-procedures/liver-biopsy/about/pac-20394576
- Model for End-Stage Liver Disease. Wikipedia, the free encyclopedia Sept 25, 2025. https://en.wikipedia.org/wiki/Model_for_End-Stage_Liver_Disease
- MELD Score. Cleveland Clinic.org Aug 14, 2025. https://my.clevelandclinic.org/health/diagnostics/meld-score
Exam Portal
click on [Take Exam]
Purchase membership here to unlock Exam Portal.
|
|
|
|
|
*Important*
Registration and login is required to place your name on your CE Certificates and access your certificate history.
Username MUST be how you want your name on your CE Certificate.