Behavior Management, A Deep Dive
Author: Mark Parkinson BsPharm: President AFC-CE
Credit Hours 4 - Approximate time required: 240 min.
Educational Goal:
Provide behavior management techniques options for In-Home caregivers.
Educational Objectives:
- Tell how social norms of behavior management do not work well in a foster care situation.
- Give an understanding of the issues that can lead to Problematic Behaviors Experienced in Care Homes.
- Tell how a caregiver must explore the root cause of behavioral problems before acting.
- Explain what the agitation response is
- Discuss various behavioral management techniques
Procedure:
Read the course materials. 2. Click on exam portal [Take Exam]. 3. If you have not done so yet fill in Register form (username must be the name you want on your CE certificate). 4. Log in 5. Take exam. 6. Click on [Show Results] when done and follow the instructions that appear. 7. A score of 70% or better is considered passing and a Certificate of Completion will be generated for your records.
Disclaimer
The information presented in this activity is not meant contraindications may be of concern. All applicable manufacturers’ product information should be reviewed before use. The author and publisher of this continuing education program have made all reasonable efforts to ensure that all information contained herein is accurate in accordance with the latest available scientific knowledge at the time of acceptance for publication. Nutritional products discussed are not intended for the diagnosis, treatment, cure, or prevention of any disease.to serve as a guideline for patient management. All procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this article should not be used by care providers without evaluation of their patients’ Doctor. Some conditions and possible
Behavior Management, A Deep Dive
 Adult Foster Care providers have a very demanding job because of the insidious and dreaded Nevers.
Adult Foster Care providers have a very demanding job because of the insidious and dreaded Nevers.
You Never get to step away from the job. You Never get to go home after work; home is work. You Never get to leave troubling and grouchy customers behind because you live with them 24/7. Even when you do get to get away, like grocery shopping, you Never get to step away from the worry. “Is there going to be a five-alarm mess to deal with when I get home? On any peaceful, calm day, a resident's troubling behavior can turn your world upside down. In order for you to survive long-term in this profession, you have to gain behavior management skills and gain them quickly. In order to gain those skills, we first have to cover a few important principles.
Thee Most Important Principle
As we grow to adulthood, we learn the social norms of how to interact with other people. Those social norms help us interact with others with a minimal amount of conflict.

For example, when working with a teenager in a group setting and the kid thoughtlessly says some stupid remarks. You can call out his name a little louder than usual and give him that look. You know the one. You can expect a normal kid to respond with, “Oops, sorry,” and things get back to normal. We have learned that if we act in a certain way, we can influence others to react in a predictable way. It comes so predictably that we take it for granted that interactions with others will always work out the normal way.
Unfortunately, our residents aren’t normal. If they were normal, they wouldn’t need us to take care of them. You cannot always get the predictable response you want. Those social cues and demands that we use just don’t work when the resident’s physical and mental state has been altered in some way. What that really means to us caregivers is that when the residents don’t act like we want them to, our normal methods of getting them to change behaviors will not work. This is thee key principle in In-Home caregiving.

Understanding it will be the difference between success and burnout, thriving or failing. If you don’t get a handle on this one principle, you’re heading for unrelenting episodes of frustration and major amounts of stress that will lead you in the end to quit. Remember the example of the misbehaving teenager. If it were a developmentally disabled teenager acting inappropriately, raising your voice and giving them “the look” would accomplish nothing. Using that tactic would only lead you to shout louder and want to physically make them behave. This in turn, gives both you and the child a lot of stress and frustration.
A Different Way
To help you get a better understanding of what I am talking about, let’s have a look at the basics of how social norms work in resolving abnormal behaviors. When different individuals interact with one another, it is expected that everyone will look after themselves and not disrupt the lives of others around them. If a person acts in a way that disturbs another person, the offended person will give social cues or a verbal request to change their behavior. Simply put, “Knock it off. You're bothering me.” It is accepted as a social norm that the offender is responsible for figuring out what they did wrong and changing their actions to get back in harmony with the offendee.
This works pretty well at resolving issues. But what happens when the offender is handicapped in some way? They are hampered in either recognizing what they are doing wrong or are unable to change, even if they understand what they are doing. The result is that stress is created, and the problem escalates.
In a care home setting, it is reasonable to assume that all of your residents are handicapped in some way that may interfere with their ability to adjust their behavior. Experienced caregivers know that they need to do things differently from the social norm. They know that they need to become familiar with the handicaps that may interfere with behaviors and help to resolve issues that may come up. You, the caregiver, are to become the facilitator of the social harmony of your home.
Issues that can lead to Problematic Behaviors Experienced in Care Homes
Maladaptive Coping Mechanisms
Maladaptive behaviors are bad habits that residents use to cope with stressors in their lives. They initially relieve the situation for the resident but ultimately cause more problems and stress for everyone.

Melissa Porrey LPC, NCC states in an article from the website Verywell health. “Maladaptive behaviors can take many different forms, but broadly fall under seven categories:
- Avoidance: This is where you intentionally steer clear of situations, activities, or thoughts that cause discomfort or anxiety, even if no threat is involved. It can lead to social withdrawal and isolation to avoid an overwhelming sense that you have no control over situations.
- Procrastination: This includes a pattern of daydreaming, often for hours on end, at the expense of current tasks and responsibilities. Chronic procrastination is often used to avoid anxiety and stress, but can end up increasing those feelings rather than easing them.
- Passive-aggressiveness: This is the pattern of indirectly expressing negative emotions, such as anger or hostility, rather than addressing them directly. It is a way of avoiding conflict, allowing you to express negative feelings without taking responsibility for them.
- Aggression: This is the pattern of "flying off the handle" with minimal or no provocation. The response can either be reactive or planned and is generally disproportionate to the situation. The pattern of aggression can disrupt relationships and fuel underlying insecurities.
- Compulsive behaviors: These are repetitive behaviors used to ease anxiety, but end up interfering with daily life and well-being. Examples include eating disorders (like anorexia or binge eating) and alcohol or substance abuse, which pose long-term harm.
- Self-harm: This includes self-cutting, burning, scratching, hair yanking, or hitting oneself in an attempt to dampen emotional pain. These actions can end up causing distress as a person is forced to hide their injuries or feels unable to control their compulsion.
- Risk-taking: This involves placing yourself in harm's way without thought to the consequences. The emotional rush may be used to replace traumatic thoughts with a false sense of elation. This not only includes physical risk-taking but also sexual risk-taking.”
Source: https://www.verywellhealth.com/maladaptive-behavior-8640911
Causes of Maladaptive Behaviors
In the same article, Melissa Porrey further states, “Maladaptive behaviors often arise from a combination of psychological, social, environmental, and even neurological factors. Some of these include:
- Learned coping strategies: These are behaviors learned from parents or caregivers who also have maladaptive behaviors. Social factors like a dysfunctional family life, poverty, neglect, or chronic stress at school or work can contribute to maladaptive behaviors.
- Prior traumatic events: Traumatic events, including assaults and sexual abuse, can lead to maladaptive behaviors as a means to avoid deep-seated feelings of pain, shame, embarrassment, or guilt.
- Anxiety disorders: Avoidant behaviors are closely linked to anxiety disorders, including generalized anxiety disorder (GAD), social anxiety disorder (SAD), obsessive-compulsive disorder (OCD), and post-traumatic stress disorder (PTSD).
- Neurodevelopmental disorders: Conditions like attention-deficit/hyperactivity disorder (ADHD) or autism spectrum disorder (ASD) are characterized by problems with self-regulation, impulse control, and social interactions, leading to maladaptive coping strategies.
- Personality disorders: Conditions like borderline personality disorder (BPD) and histrionic personality disorder (HPD) can manifest with emotional outbursts and poor emotional regulation due to underlying feelings of inadequacy or an intense fear of abandonment.
- Neurological conditions: A traumatic brain injury or stroke can cause marked changes in behavior, including impulsivity, aggression, and anosognosia (a lack of awareness about risks).
| Medical Conditions |
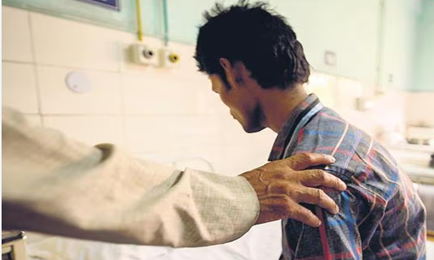 |
There are many illnesses, disorders and injuries that can affect the function of the resident’s brain. These can lead to changes in awareness, movement, and behaviors. They can cause a normally acting resident to suddenly misbehave. No amount of corrective actions from the caregiver will remedy the situation until the underlying condition is addressed.
|
Central nervous
System issues
|
Brain bleed (hemorrhage)
Brain tumor
Hepatic encephalopathy
Fluid build-up in the brain
Seizure
Stroke
Traumatic brain injury
|
|
Metabolic disorders
|
Dehydration.
Hypothermia.
Hypoxemia (Low blood oxygen)
Hypoglycemia (Low blood sugar)
Hyponatremia (Low sodium levels in the blood)
Hypocalcemia (Low calcium levels in the blood)
Hypothyroidism (Underactive thyroid)
|
|
Drug side effects
|
Antiseizure medications
Anticholinergics (a group of drugs that control involuntary muscle movement)
Corticosteroids
Sedatives
Sleeping pills
Overdose or withdrawal of addictive substances
|
|
Infections
|
UTIs
Encephalitis
Meningitis
Pneumonia
|
 Loss of Mental Capacity
Loss of Mental Capacity
Any condition or combination of conditions that reduces the ability of the brain to function properly will understandably lead to problematic behaviors. Often, the resident is unaware that they are causing problems. Expecting normal behaviors or reactions to caregivers' demands is unrealistic because they have lost the mental capacity to do so.
These conditions include
Pre-existing personality and psychiatric illnesses
Being Developmentally Disabled
Diseases that affect the Brain (Alzheimer's, Parkinson’s, Cirrhosis, Chronic drug Abuse, Age-related conditions)
Reduced vision problems that can cause hallucinations
Here is a good YouTube video that shows you what that might look like.
Disclaimer- I have no financial connection to any of the videos used in this lesson. I did not produce them. I found them in YouTube's public domain. Please forgive the commercials. They enable me to give you the material for free. If you want to look further into the presenters' programs, contact them directly using the information provided or look in the comment section below the video.
Loss of the Ability to Communicate Properly
The resident who cannot communicate properly will naturally be under more stress. This inability to communicate leads to unmet biological and emotional needs. The only way to get what they want is to act out to get your attention. If there is additional cognitive decline, the resident will act out without knowing why they are agitated. For example, there might be a pain issue or a need to go to the bathroom that leads to aggressive or inappropriate behaviors.
Here is another excellent YouTube video dealing with issues related to loss of language skills. The presenter explains the biological cause of some bad behaviors related to dementia. Please excuse the bad language; it is appropriate in this example because you might face it yourself someday. It’s a long video, but trust me, it’s worth it. There will probably be a test question or two from the video.
Acting on the Principle: Stop and Look Deeper
The takeaway from all of the above is that there could be many reasons for bad behavior in your residence. There is a genuine possibility that they may not be able to help themselves from acting badly. There is also the distinct possibility that the patient may not be able to correct the disruptive behaviors once they happen. There are too many factors that may not be under their control. In care homes, the occurrence of these circumstances is so prevalent that In-home caregivers must learn a new way of dealing with problem behaviors. As you probably have already experienced, the old social norm ways of correcting bad behaviors just lead to worsening conditions. In-home caregivers must learn a new way of handling problem-causing situations.
Let’s call this new way the Stop and Look Deeper method. Stop and think before reacting. Look deeper into what may be causing the conflict.
This may seem like a daunting task, given all the different things that could be happening. In reality, it’s not that hard. All you have to do is get to know your residents well enough to be able to see the situation from their point of view, while taking into account all their handicaps. Some may call this empathy; I just call it well-informed good caregiving.
So, in the Stop and Look Deeper method, the first step is to never assume that the resident can change their behavior just because you ask them to. The second is to always ask yourself, Why are they acting abnormally, before responding. Now, this does not mean to start treating the resident as if they were incapable of handling themselves. What it does entail is that you know what issues may arise in advance and be ready to head them off before they become a problem. It also requires you to always be ready to help your resident adjust their problem behaviors using the tools in your caregiver toolbox. We’ll cover that later.
The Second Principle: Aggravating Circumstances
An agitated resident is one of the most concerning abnormal behaviors that In-Home caregivers have to deal with. We try are best to suppress the bad behavior but our efforts seem to be pouring fuel on the fire. The situation quickly escalates to one of those 5 alarm messes that we so dread. In desperation, caregivers give up and reach for sedating medication that seems to take forever to calm the patient.
The paradoxical truth of the matter is that most of the time, trying to suppress the agitation only aggravates the situation, causing more agitation. When we give up and reach for sedating drugs, the underlying cause is still remains. So you have to fight with the patient to take the drug, which makes the situation worse. Then you have to endure the five alarm condition even longer, waiting for the medication to kick in. And what about the side-effect concerns you have to deal with? It hardly seems worth it. I hope it is self-evident by now that if you just concentrate on suppressing the agitated behavior, everyone ends up being frazzled way more than you ever wanted. So the second principle to learn is that you have to understand what agitation really is and avoid the things that make it worse before you try to control the resident's bad behavior.
Acting on the Principle: Respond to the Stressor, not the Behavior
Everyone experiences agitation sometimes in their life. Think back to when you were agitated. What helped you more? 1. Someone telling you to calm down and shut up, or 2. Someone listening to your concerns and helping you resolve them? Well Captain Obvious, I’ll think I’ll take option 2. So the first step in controlling the agitated behavior is to find out what is triggering the agitation in the patient in the first place. This may seem like another Captain Obvious question, but is it really? Do residents always know what’s bothering them? Hardly. Even if they knew, can the resident always communicate with you clearly when they're upset and agitated? In care homes, the answer is almost always No.

So what is a caregiver supposed to do, turn into Sherlock Holmes? Elementary, my dear reader….Yes. First, you have to understand what agitation is and what triggers it. Then look for those triggers in the surrounding environment and try to control them. The next step is you have to investigate the actions and the responses of the resident. Doing both steps will help you gain the clues you need to help them in a way they will understand and cooperate with. Then the bad behavior resolves itself. No 5-alarm fires, no need for sedating drugs. The end result- quicker and easier resolutions.
What Exactly is the Agitation Response
The exact biological mechanisms that produce agitation are not fully understood yet. There are many chemical pathways involved that affect the amygdala portion of the brain, which may, in turn, create the agitation response. Generally speaking, though, agitation is an automatic protective response to a stressor. The body is notifying the brain that something is wrong. The brain then starts ramping up the body, getting ready to act to relieve the stress. The more stress that is experienced, the more agitated the patient becomes.
|
Internal signs of agitation
|
Outward signs of agitation
|
|
Irritability
Tension
Mental distress
Restlessness
|
Being uncooperative
Clenching fists or wringing hands
Difficulty focusing
Excessive talking
Fidgeting
Hostility.
Inner restlessness
Lack of impulse control
Pacing
Violent or disruptive behavior
|
|
The levels of intensity usually start out as mild occurrences in response to some unfulfilled need or experienced stressor. Because of the automatic nature of the response, patients may not even notice the symptoms of agitation that are starting to occur. If the need remains unfulfilled, the agitation continues. But if conditions in the environment or caregiver reaction add to the stress, the agitation escalates to a moderate condition, and then continues to severe. In severe cases, the agitation response usually overcomes rational thought. The only thing that matters is relieving the stress. Caregivers find it extremely hard to reason with the patient from then on. It’s like all portions of their brains have turned off except for the parts dealing with the stressor.
So the caregiver has to go into that place and pull them back from the brink. (Well cover those techniques later on as well.)
|
 |
Aggravating Circumstances
Let’s have a conversation about what may trigger the agitation response in our residents. Once you become familiar with them, you will know what to look for. Knowing what to look for is half the battle won.
Lower the Trigger Thresholds
Because chemicals and brain structures are involved, there are many drugs and medical conditions that can produce agitation symptoms. Making the patient more susceptible to reocurring episodes.
|
Medical Conditions
|
Medications
|
|
Delirium
Dementia/ Alzheimer’s
Infections (like UTIs), especially in people over 65
Electrolyte imbalances
Hyperthyroidism
Physical trauma, especially head trauma
After Seizures
Substance intoxication or withdrawal (alcohol, nicotine, marijuana, hallucinogens, and opioids)
Toxins (poisoning)
Autism spectrum disorder
Anxiety disorders
Bipolar disorder
Depression
Schizophrenia
|
Medications with caffeine
- Migraine Meds (Excedrin, Anacin, Cafergot)
Corticosteroids
- Cortisone
- Dexamethasone
- Prednisone
- ADHD drugs
Amphetamine/dextroamphetamine (Adderall)
Dexmethylphenidate (Focalin)
Lisdexamfetamine (Vyvanse)
Methylphenidate (Concerta, Ritalin)
Asthma Medication
- Albuterol
- Salmeterol
- Theophylline
Thyroid Medication, Seizure Drugs and Parkinson's Disease Medicine
|
It may seem like a long list, but that does not make it difficult to handle. It is just a matter of holding up the list next to your resident and seeing if they have factors that increase the risk of agitation. Once you determine they are at increased risk, there is less likelihood of being taken by surprise by agitated behaviors. You can be better prepared to act quickly to keep the agitation in the mild stage.
Investigation Starts the Intervention
There are so many variables that can create tension or strain your residents that it’s not very effective to assume you know what’s going on before you intervene. When incidents of agitation start to occur, just like the famous detective Sherlock Holmes, you have to start the investigation by gathering the clues. Once you have gathered enough evidence, your interventions will be much more effective. And just like a detective, your investigation will be much more efficient if you start with the usual suspects.

Internal Stressors
Any need the resident has that goes unfulfilled strains the patient and becomes a stressor. Diminished abilities like the inability to communicate, cognitive impairment, or vision loss make it harder to take care of those needs. That adds to the patient’s frustration. The greater the disability, the more frustration is felt, and the greater the agitation that is manifested. Therefore, recurring needs like pain relief, hunger, bathroom breaks, boredom, depression/sense of loss, mania, allergies, worry, and loneliness become the “usual suspects” when you start your investigation.
External Stressors
Having to deal with things we don’t like is an automatic stressor. In addition to that, the brain only has a finite amount of ability to process input from its surroundings. Exceeding that limit is also a stressor. When disability further reduces the ability to process input, everyday things like colors, patterns, noise, commotion, and odors become the “usual suspects” to start investigating. And don’t forget changes in the environment, routines, or people interacting with the resident can readily set a person on edge. So ask, what has changed that is causing the agitation?
Caregiver Caused Stressors
Unfortunately, one of the usual suspects that causes agitation is the Caregiver themselves. Isn’t it ironic that the one person in the room who is trying to reduce the agitation may inadvertently be adding to the stress of the situation? Don’t feel too bad about though. No one comes into this business fully trained. You have to gain experience on the job or get some training in another medical field. Some of the things I have noticed In-Home caregivers doing that stress out the residents are;
Treating the resident like a child or a problem that is annoying the caregiver.
Reacting too loudly, too positively, too quickly
Saying one thing and acting another.
Not listening to the patient, disregarding what they are saying or dismissing their concerns out of hand.
Acting against them, not for them. Not seeing things from their point of view.
- Making the residents feel inferior
Making the patient feel that the rules are more important than the patient.
- Letting yourself become agitated
When you lose your cool, everything you do, good and bad, becomes an aggravation, making things worse.
All of the above can be really irritating to a stressed-out patient. They can negate any good that you are trying to do. The usual result is instead of calming the patient, you quickly escalate the agitation to higher levels.
Let’s do a practice exercise. Put on your Sherlock Holmes hat on and look at this video. List the items that you see that may be contributing to the patient's agitation.
I listed the stress of unresolved pain, Nicotine withdrawal, the stress of being in an unfamiliar hospital setting with uncomfortable clothes on, and people who are strangers telling her what she can’t do. The caregivers are not really listening to her. Telling her that hospital policy is more important than her needs. They say they are trying to help but their body language says they are there to control here. What did you come up with?

Being Sherlock
There are better ways to handle agitated residents that don’t lead to 5-alarm fires. Let's call it the Supportive Sherlock Holmes method. Instead of trying to suppress the agitated behavior, you concern yourself more with what is needed. Instead of acting, you begin by investigating. What is causing the issue? Is the resident at greater risk for higher levels of agitation? Is there something in the environment that is aggravating the agitated patient? Does the resident have a need that needs attention? Are my actions helping or making things worse? Once you begin to be Sherlock, you will notice that events stay under control more easily. You will have less surprise 5-alarm fires to put out. Your stress level drops, and you don’t get burned out. Much better, yes?
Behavioral Management Techniques
There is no one best way to handle behavioral problems. It is a matter of learning several techniques that fit your style of care and using them as the situation requires. I like to use the analogy of tools in a caregiver's toolbox. Some tools you’ll use almost every day. Others only as needed. The following are techniques for you to consider adding to your toolbox.
 Discreet Assessment
Discreet Assessment
Behavioral management has two distinct phases: assessing and acting. Investigating the causes is essential but doing it the wrong way can aggravate the situation in so many ways. Use tact and discretion to avoid making the problem worse.
- Visually assess the overall environment. Make mental notes of what the possible stressors are.
- Focus on the person. Pull up your mental files on the resident. What are the predisposed risks and normal behaviors? Then ask what is different? Start with the usual suspects and form a hypothesis. Then start asking questions to confirm your guesses.
- Ask questions as a caring advocate, not as an enforcer of the norm. For example, “Hey Hal, I see that you’re troubled. What seems to be the problem? Are you in some pain?” Not, “What's going on in here, Greta? Are you fidgety because you need to go to the bathroom?”
- Remain flexible in your investigation. Don’t jump to any conclusions. See the problem(s) from the patient's perspective as well as your own.
- Decide if it even matters. Some battles are just not worth fighting.
Now you're ready to act wisely, and the resident sees you as a helper, not as a judge and jury or a foe.

Professional Armor
You are the professional caregiver here. It’s your job to calmly take care of your patients. It’s not the patient's job to make you feel good. You are ultimately responsible and in control of the home. Use that professionalism as a layer of armor so that nothing gets under your skin. It will help prevent you from responding emotionally and becoming a stressor.
Patient’s Perspective
Your residents are patients. They have conditions that handicap them and prevent them from perceiving the world as you do. They cannot come to where you are mentally and or socially. You have to go to the world that they exist in. If a person has a wheelchair, you don’t give them tasks that require standing or walking. You alter the conditions so that they can accomplish the task while sitting in the wheelchair. In behaviorally handicapped patients, the same adjustment of conditions needs to be done. But in these cases, you are altering your communication style and the content of what is said to fit the world that they live in.
For an example of what I am talking about, watch this video about Dementia patients wanting to go home.
At first, this concept is difficult to understand conceptually. Unlike a physical handicap, you cannot readily see mental and or social impediments. But once you comprehend that they are almost communicating in a different language. (similar to the one you use, but based on comprehending circumstances differently), interacting with them becomes easier.
This caregiver tool requires practice on how to use it effectively. It may feel like you are lying or manipulating the resident. Socially, you are conditioned to see this as a bad thing. That is not what you are trying to do. You are not conning them; you are acting as an interpreter. You are presenting concepts in a way they will understand. In the video example above, telling the patient that they can’t go home because of exterminator fumes is actually telling them it would be emotionally difficult for them to see that you can never go back to the way things used to be. I like the label of therapeutic fitting the presenter used. You are helping the handicapped patient fit into the real world in a verbally therapeutic way. Once you become proficient in this communication therapy, other caregiver tools become more effective.
Positive Paradigm Approach
Another caregiver tool that makes other tools more effective is having a positive attitude toward everything you do as a caregiver. The human psyche has two sides. A rational side that deals with facts, logic and outcomes (The thinking side) and an emotional side that deals with feelings. We start out in life with feelings being prominent. As we learn to think for ourselves, the rational side becomes more and more prevalent. The rational side ends up governing the actions we take. When the thinking side is compromised in some way, the emotional side takes over and governs the actions we take.
That is why those residents who are mentally or emotionally handicapped are more easily triggered.
In addition, emotions color our interpretation of the facts. Negative emotions only see the trials of events and facts; positivity sees the opportunity in situations.
Positivity affects behavioral management in four ways.
- Approaching caregiving in a positive mindset enhances your professional armor. Situations and troubled residents can’t get under your skin and provoke a negative response from you.
- Positivity prevents the caregiver from becoming a stressor and aggravating the agitated resident.
- It makes it easier to see the opportunities in interactions. You will see openings to de-escalate a crisis sooner, see avenues of redirection faster, and come up with substitution ideas quicker. It enhances your creativity in solving problems.
- If you are consistent with your positive approach, the patient learns to see you as a helper and a solver of problems. Trust is built, and they will more readily accept and comply with your suggestions.
De-escalation
In the middle of a 5-alarm situation, the resident is in a crisis mode or escalating towards it. The emotional side of the brain has taken over and is not listening to reason. If a caregiver tries to intervene by using rational arguments, the resident will likely resist them and be agitated by your attempt to help. The very effort to solve the situation can escalate the situation into further conflict. A De-escalation is needed before trying to resolve the problem.
Effective de-escalation is accomplished in several general steps.
- Reduce or eliminate aggravating elements. Separate those who are arguing. Reduce unneeded noises and distractions. Ensure safe conditions for all involved, including the caregiver. Have a clear avenue of escape.
- Calm yourself before entering into the crisis. Present yourself in a positive, neutral manner. Hint- Slow, deep cleansing breaths help.
- Approach the patient on their dominant side. They will feel in control from that side. Do it in a way that will not startle them. Stand away from the resident, providing a safe, non-threatening space.
- Get the person's attention without touching. Get eye to eye with them, even if you have to crouch.
- Do not tell the patient to calm down. Instead, start an investigation conversation with the resident. (For example- “I want to help, but first I need to understand. Tell me what is going on.”) Talk in pleasant, calm tones with a smile on your face. Then just listen to their response. Pay particular attention to the emotions that are in play.
- State back the emotions that you mentally listed, then ask them if you got the list right. For example.
- “I see that you are feeling angry and disrespected. You feel that nobody cares about how you are feeling and feel abandoned. Did I miss anything?”
- “I sense that all the commotion is making you feel confused and that is making you feel insecure. Is there anything else that you are feeling?”

Talking first about the feelings being felt provides an avenue of release for the pent-up emotions. It validates the emotions, confirming that you understand why they are acting out. It also forces the rational side of the brain to start thinking in terms of facts and conditions. Often, the patient doesn’t even know what they are feeling until you give them a label. It also shows the resident that you are really trying to understand, and there is no more need for aggressive behaviors to get your attention.
Helpful Hints
- Look for non-verbal clues that will help you determine the emotions that they are feeling.
- Eliminating the audience prevents embarrassment complications. Ask everyone to leave or walk the resident away to a secluded spot.
- The act of walking side by side is calming.
- Be aware of your own body language. It may be the only language that the resident is hearing at first.
- Offer a piece of gum to chew or a sweet snack to eat. Chewing sends calming messages up the vagal nerve to the brain. The activity also distracts away from the tensions being felt.
- After (not before) the resident starts calming down, suggesting deep breaths may speed up the process.
- Touching the resident (like a hug or shoulder rub) should only be done with their permission after the calming process has begun.
Once you see the resident is more in control of their emotions, you can proceed with other tools from your caregiver toolbox.
Substitution
In Substitution, caregivers suggest an alternative to fulfill the need that provides an advantage over what is currently being sought by the resident. (You’re giving them choices in what they can do, not dictating what they can’t do.) It could be a favorite physical object or an alternative idea or method.

For example:
- Offer to trade a cookie for a TV remote control.
- Offer a doll or something that provides security to someone who is full of anxiety
- I see what you are trying to do, but I don’t know why it’s not working (causing difficulties, breaking things etc…). Point out the difficulties the idea is causing. You have done this in the past, and it seemed to have worked. Why don’t you try that? Make it appear that they came up with the idea.
- I agree with you in principle, but don’t you think that (alternative) would (point out benefit) be a better way?
- I see the need now that you pointed it out. But I am feeling under the weather today. Could you help out a tired old lady and do me a favor and try this instead? (When they pause to consider the idea, say) Oh thank you, you're such a good friend. I will return the favor someday.
Helpful Hints
- Liberally use therapeutic fitting in these cases. They are trying to accomplish something; frame your alternative as the solution to what they are trying to do using the very ideas they are saying. “I see now, thanks for pointing it out that (fill in blank). I never would have thought of it that way. I think that (fill in alternative) would do nicely to solve the problem, don’t you agree?”
- Guide the conversation in steps so that the patient chooses the alternative approach.
- Praise them for figuring out a better way of working on the need and or praise them for accomplishing the task at hand, providing closure for the problem behavior. Nobody argues with someone trying to give them a compliment.
- Frame the alternative as a special talent that the resident does in a particularly good way.
Here is an example of substitution
Redirection
In redirection, you are trying to make a clean break from the problem behavior by diverting attention to another activity. The alternative activity has to be distracting or entertaining enough to divert the attention of the resident. This tool can be used like a magician to pull away the focus of the resident away from what you are doing behind their back, or it could be used like a traffic cop turning the flow of the action in a new direction.
- I like that dress (dirty laundry that needs to be washed) but Oo I like that dress even better. (making another choice seem more desirable) That will do much better for the weather we are having (or any other event/quality that gets their attention off the dirty dress). Please be a dear Hun and place that dress in the laundry. That will help me so much, I’m so busy today. (redirecting from dressing to helping with chores) Let’s hurry now, I’m making waffles this morning, and you don’t want to miss that. (changing the subject from dressing to eating a favorite food). This is taking too long, the others are going to get mad about having to wait for their waffles, and we don’t want that (redirection attention from self to others judging her) let me help you to speed things up. (changing the focus from selecting clothes to how fast the task is taking)
Diverting Attention
Diverting the residents' attention away from problem topics and situations may seem like a Captain Obvious thing, but I find this tool is harder to pull off than other techniques. In my opinion, it should only be used at the early stages of the problem. Since diversions do not address the underlying stressors, when tensions are higher, those efforts may be interpreted as overt manipulation and actually cause more conflict. I recommend you watch this video; she has some really good techniques that you could use in your care practice.
To help you be more effective in problem-solving, I suggest you have a variety of preplanned distraction activities prepared that address common concerns of the resident.
- Simulated presence therapy (use of videos or audiotaped recordings of family members)
- Reminiscence therapy (discussion of past experiences)
- Favorite snacks
- Walks (one of my favorites)
- Quite room with something in action, like a fish tank, videos, music, a puzzle, or computer games.
- People like to help and feel useful, especially bored clients. You are not taking advantage of free labor if you are using it as a moral booster. Chores are most effective when followed by sincere gratitude and praise.
- Comfort items like a doll, stuffed animal, or favorite book (Bible).
Replacement Behaviors
Of course, the most effective therapy is to solve problems in advance. For recurring problems with known solutions, altering long-term behaviors to meet needs is worth the effort. Long-term behavioral changes have to be internally motivated and can be facilitated with caregiver support.
Supportive caregiver actions:
- Scheduling activities with the goal of creating habits.
- Clearly stated expectations that are often repeated
- Providing visuals/pictures. Both on the wall and in laminated handouts, and even in repeated computer videos.
- Elicit help from family, friends, and authority figures like clergy or medical professionals.
- Include the resident in planning schedules and activities. Create ownership in the patient.
- Reinforce changes in behavior with sincere praise and validation statements given often.
- Aromatherapy (use of fragrant plant oils)
- Cognitive behavior reinforcement conversations. Talking about the “Why” reasons of actions and utilizing the power of positive thinking.
Periodic assessment will be required. Compare what you think is going to happen with what is actually happening. Take note of what works and what does not. That list will be helpful to you in other circumstances.
Reinforcement Activities (Yes, I am using behavioral modification tools on you.)
Take note of the different techniques that are used in the following video.
How could you adapt the techniques used in this video to your care home?
Here’s another good training video
Conclusion
Trying to modify troubling behaviors in our residents the same way we interact with the general public is not a very effective way to handle troubling situations. Relying on drugs is often too slow and comes with additional side effects to deal with. In my experience, there are better techniques for handling problem behaviors.
- Discretely look for issues that can lead to problematic behaviors before trying to solve problems.
- Investigate as you intervene. Become a Sherlock Holmes
- Know what risk factors for altered behavior your residents have.
- Use your protective armor so that through your professionalism you can maintain control and do not aggravate the situation.
- Use positivity to make your efforts more effective.
- Use purposeful de-escalation techniques
- Develop your own substitution, redirection, divert attention, and long-term replacement techniques.
At first, it may seem like you're lying to, manipulating, taking advantage of your residents. But as you become skilled in their use, you will see that you are, in fact, benefiting your residents and keeping them happy. Happy residents equals easier caregiving.
And as always, Good luck in your caregiving efforts. Mark Parkinson BsPharm.
References:
- Malissa A Mulkey, Cindy L Munro. Calming the Agitated Patient: Providing Strategies to Support Clinicians. NIH, National Library of Medicine. PubMed Central. PMCID: PMC8171292 NIHMSID: NIHMS1697787 PMID: 34092999. Published in final edited form as: Medsurg Nurs. 2021 Jan-Feb;30(1):9–13. https://pmc.ncbi.nlm.nih.gov/articles/PMC8171292/
- Wendy Boren, BS, RN. How to Deal With Difficult Behaviors. Quality Improvement Program for Missouri University of Missouri-Columbia. chrome-extension://efaidnbmnnnibpcajpcglclefindmkaj/https://nursinghomehelp.org/wp-content/uploads/2023/12/How-to-Deal-with-Difficult-Behaviors.pdf
- Cleveland Clinic.org. Jun 24, 24 https://my.clevelandclinic.org/health/symptoms/agitation
- Michael D. Jibson, M.D., Ph.D. How to Reduce Acute Agitation in Your Patients. Psychiatry online. Psychiatric News Volume 54, Number 17. Aug 29, 2017. https://www.psychiatryonline.org/doi/10.1176/appi.pn.2019.8a16
- Persons with Dementia: Skills for Addressing Challenging Behaviors. Education for Rural and Underserved Communities. Apr 8, 2016. https://www.youtube.com/watch?v=hgVMKEnkvHo
- Caregiver Training: Agitation and Anxiety | UCLA Alzheimer's and Dementia Care Program. UCLA Health. 2018. https://www.youtube.com/watch?v=hahvUXwTXE4
- Tips On How To Calm Down Someone Who Has Dementia.
- Senior Safety Advice. 2021. https://www.youtube.com/watch?v=GZOkQyIqvEs
- Teepa Snow. Time with Teepa: How Can We De-escalate Someone That is Agitated? Teepa Snow's Positive Approach to Care. 2023. https://www.youtube.com/watch?v=2kMjA5z8XAg
- Teepa Snow. How Dementia Affects Language Skills. Dementia - Redirecting Hallucinations with Teepa Snow of Positive Approach to Care. Teepa Snow's Positive Approach to Care. 2019. https://www.youtube.com/watch?v=3s0ktYUIn0Y
- Dawn-Elise Snipes PhD. 10 Tips for Verbal Crisis De-Escalation and Intervention | Communication Skills Improvement. Doc Snipes 2021 https://www.youtube.com/watch?v=ra_Lq0DbkiM
- Teepa Snow. Supporting Changing Abilities While Keeping Her Safe in the Kitchen - Mid Dementia. Riverside Health. 2024. https://www.youtube.com/watch?v=1XR1Fzv6uFs
Exam Portal
click on [Take Exam]
Purchase membership here to unlock Exam Portal.
*Important*
Registration and login is required to place your name on your CE Certificates and access your certificate history.
Username MUST be how you want your name on your CE Certificate.